UT-Led Team Working on Improved Hydrocephalus Treatment
Highlights
- Hydrocephalus is caused by excess spinal fluid in the brain
- One million Americans have this potentially fatal condition
- TerMaath has developed a new shunt to ease symptoms
- In the News: Building a better brain shunt
- Video: UT’s Stephanie TerMaath explains the research her team is doing on brain shunts
A team of researchers led by Stephanie TerMaath, UT’s Jessie Rogers Zeanah Faculty Fellow, is making promising strides in the treatment of hydrocephalus, a debilitating and sometimes fatal condition caused by an excess of cerebrospinal fluid surrounding the brain and spinal cord, by engineering an alternative to a device currently used to relieve symptoms.
“There’s no cure for hydrocephalus right now, only treatment of the effects through a surgically implanted device called a shunt,” said TerMaath, of the Department of Mechanical, Aerospace, and Biomedical Engineering. “Unfortunately shunts have a high rate of failure, requiring more surgeries for revision. We’re developing a new ventricular catheter that will be more resistant to obstruction, a common cause of shunt failure.”
Cerebrospinal fluid provides immune support, regulates circulation, and cushions the head and spine. However, if that fluid fails to be absorbed naturally or if an excess is produced, it can cause severe problems with vision, coordination, and mental abilities, and, if left untreated, can lead to death.
According to the Hydrocephalus Association, one million Americans suffer from the condition, and its appearance rate in newborns—once in every 1,000 births—makes it as common as Down’s syndrome and more prevalent than spina bifida or tumors.
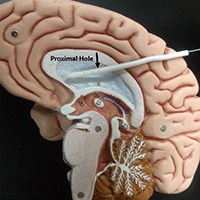
The catheter will be designed for optimal fluid flow dynamics that minimize the likelihood of both internal and external blockages.
TerMaath joined with assistant professor and fellow department member James Coder, Taylor Erwin and Ryan Glasby from the UT-Oak Ridge National Laboratory Joint Institute for Computational Sciences, and UT Medical Center neurosurgeon James Killeffer to form a multidisciplinary team to address all aspects of the project, from computational modeling to surgical implantation.
Their approach has gained them national recognition—the National Institutes of Health is now funding the research through an R15 grant—but the project also hits home on a more personal level.
“Many members of our team, including the students, either have an implanted shunt themselves or have a family member who does,” said TerMaath, who has undergone six brain surgeries in the past 10 years. “The onset of symptoms due to shunt failure is so sudden that one moment you can be fine, and the next you can be in the operating room.
“Our team understands the debilitation that accompanies hydrocephalus, and that serves as even more motivation.”
For those suffering from hydrocephalus, it offers something else: hope.
Contact
David Goddard (865-974-0683, david.goddard@utk.edu)
